TrelCor Bone Formation
Bone regeneration is a cellular driven process that can be affected by a bone graft material. The basis for Biogennix TrelCor technology was to combine multiple advanced features to enhance and improve the cellular response. With a nanocrystalline HCA surface and a biomimetic pore architecture, TrelCor bone grafting products provide an enhanced environment for bone formation.
How Does TrelCor Technology Enhance the Bone Healing Process?
Immediately following implantation of TrelCor bone grafting material, osteoblasts migrate into the porosity and attach to the nanocrystalline surface. This is followed by in-growth of blood vessels through the bone graft structure.
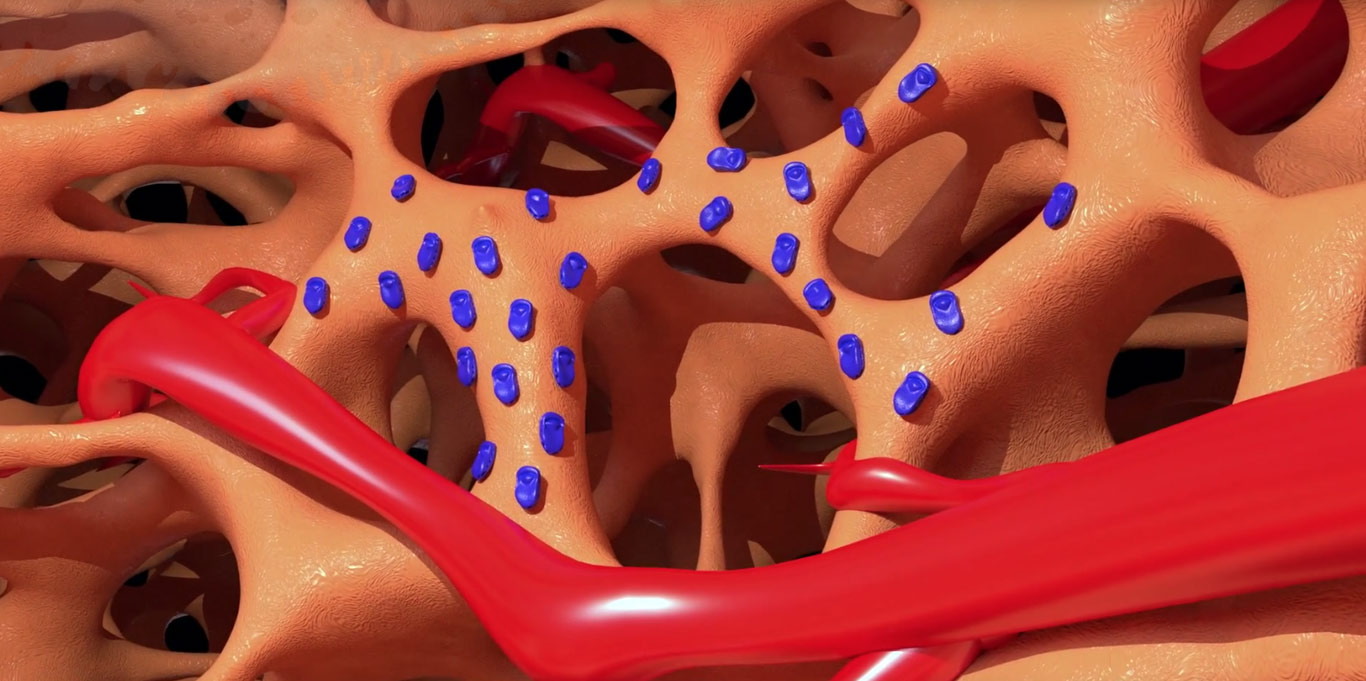
Over the first several months, osteoblasts grow, proliferate, and form new bone directly on the surface of the TrelCor bone grafting material.
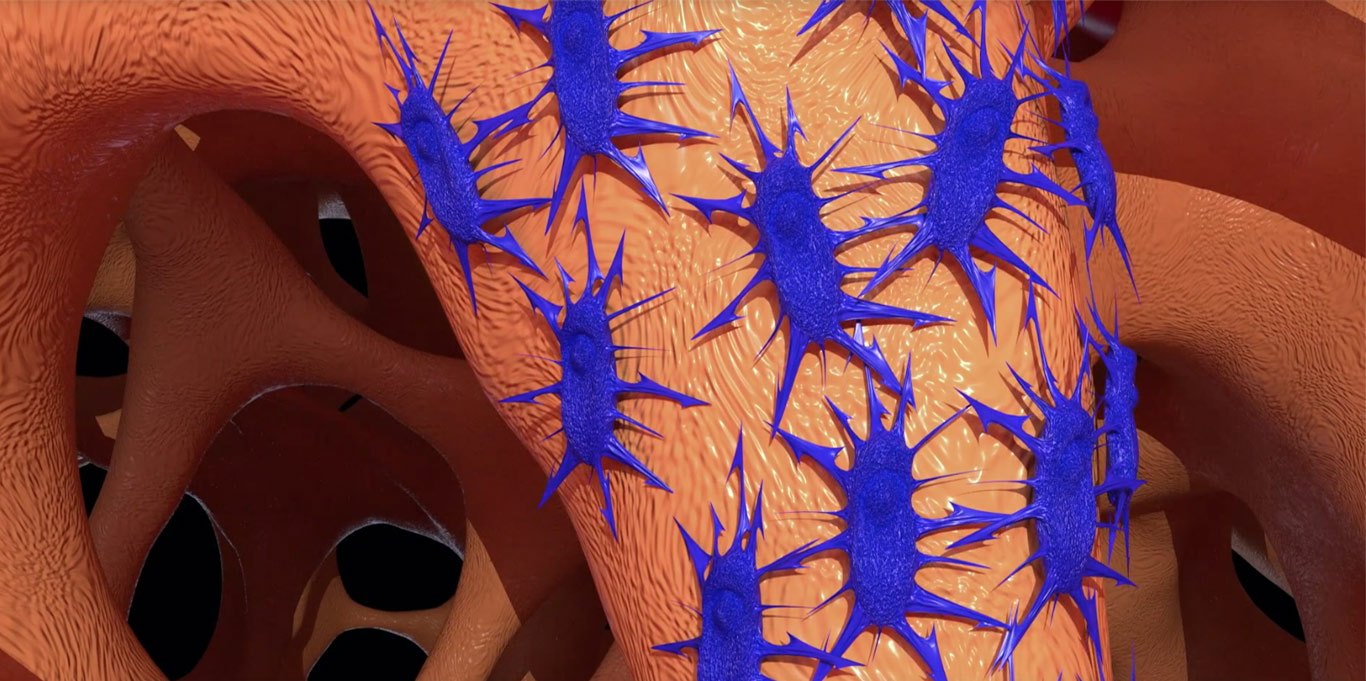
At the same time, osteoclasts (red) attach to the HCA surface, penetrate, and begin resorption of the underlying calcium carbonate core. As the calcium carbonate is resorbed, osteoblast (blue) begin to lay down new bone.
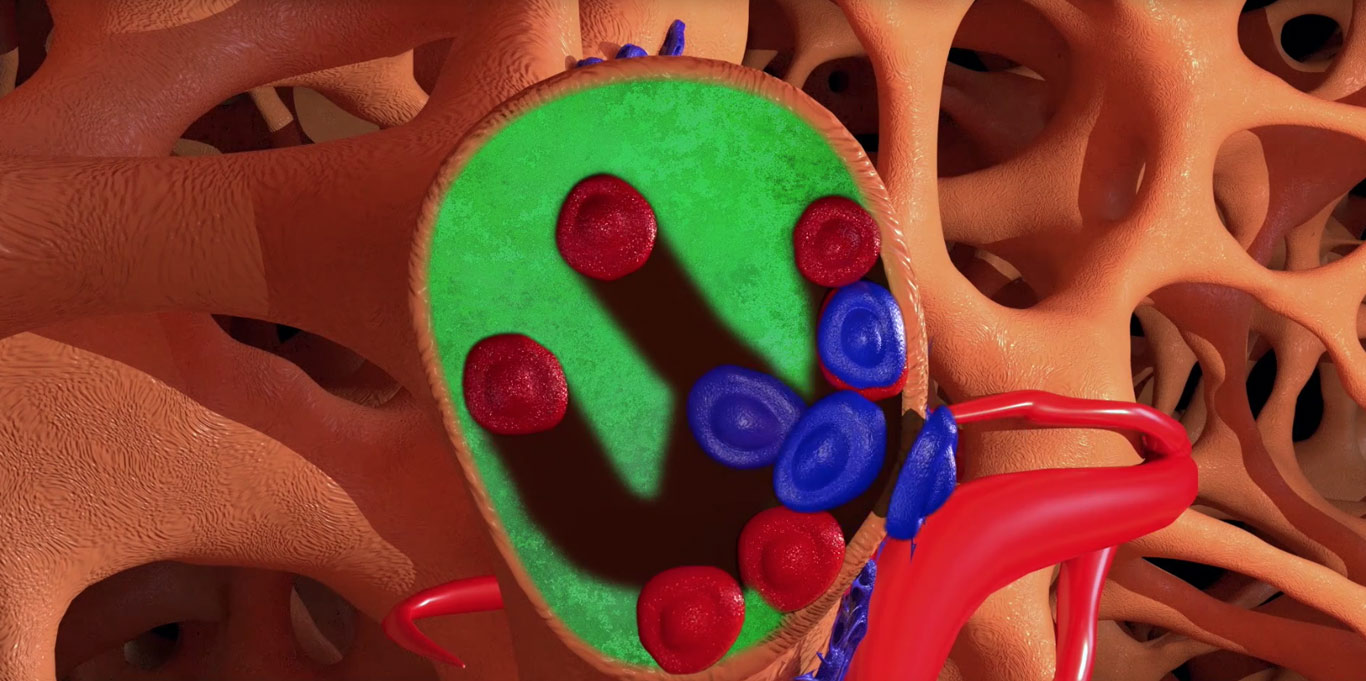
The TrelCor granules are eventually completely resorbed and replaced with mature bone.
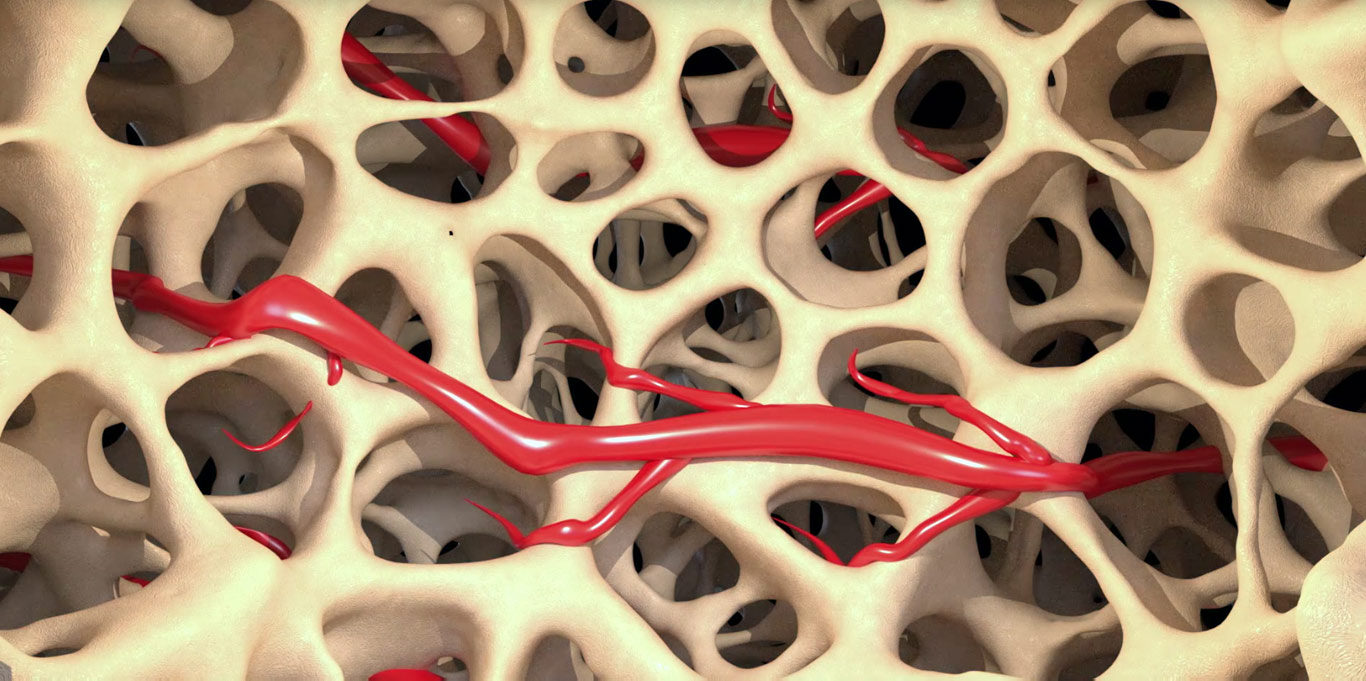
In Vivo Posterolateral Fusion Study
The bone forming ability of TrelCor was evaluated in a rabbit posterolateral fusion study.1 In the study, TrelCor granules in an organic binder were implanted with autograft in the posterolateral region of the lumbar spine. Bone formation was assessed at 6- and 12-weeks using histology, histomorphometry, microCT, and scanning electron microscope (backscattered imaging; SEM-BSE). A fusion assessment was conducted to determine the presence of continuous bone across the transverse processes (TPs).
The results at 6-weeks showed bone formation directly on the surface of the TrelCor granules and through the interconnected porosity. Continuous bone was also seen growing across the granules with progressing fusion apparent in all animals. By 12-weeks, the microCT fusion assessment showed continuous, bridging bone across both transverse processes (Figure 1). Bone was seen growing off the transverse process and into the granule porosity. Bone was also seen growing between the granules which resulted in continuous, bridging bone that spanned both TPs.

FIGURE 1
Isometric Micro-CT view of
TrelCor granules in the rabbit
posterolateral spine at 12-weeks
Continuous bone is seen bridging the
transverse processes
The histology and histomorphometry results showed that bone formation continued to increase from 6 to 12 weeks. Histology at 12-weeks showed mature bone surrounding the TrelCor granule. Resorption was also evident with new bone growth penetrating through the HCA surface into the calcium carbonate regions (Figure 2). Before TrelCor resorption occurs, the thin layer of HCA (white layer in the image) covers all the surfaces of the TrelCor granules. As seen in Figure 2, resorption at 12-weeks has resulted in intermittent breaches of the HCA surface (segmented white line). This has allowed regenerated bone (yellow) to replace a large portion of the underlying calcium carbonate core.
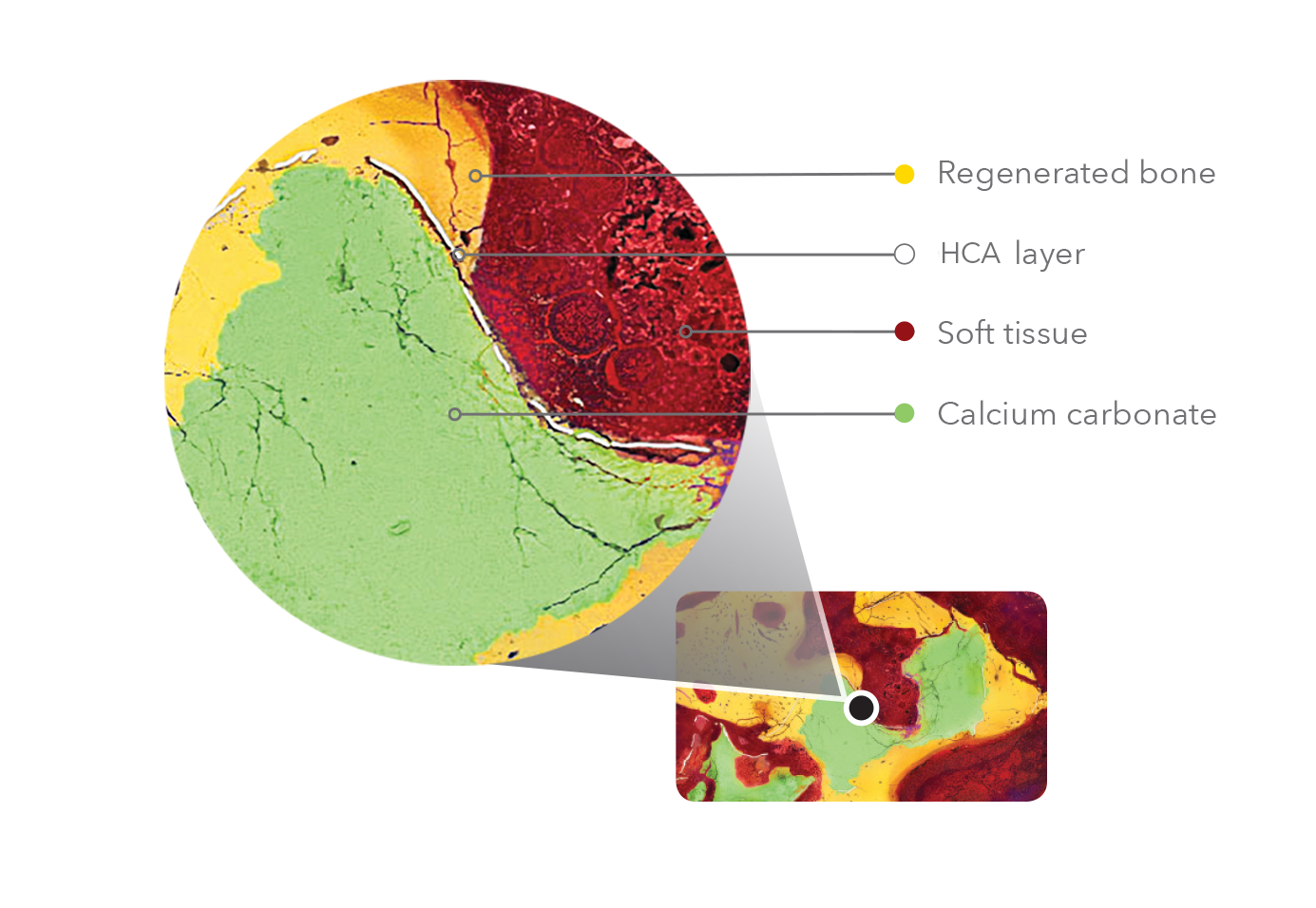
FIGURE 2
SEM-BSE
(false-colored) image
of TrelCor granules in a
posterolateral spine
Overall the results of the study show that TrelCor bone grafting material combined with autograft was able successfully fuse the rabbit posterolateral spine. Bone formation was evident at 6 weeks and increased by 12 weeks. The TrelCor granules supported bone growth on the surface, in the porosity, and in between adjacent granules. Resportion was evident at 12 weeks with new penetrating the HCA layer and replacing the underlying calcium carbonate core. The results showed that TrelCor was an effective bone graft material.
References
¹ Data on file at Biogennix